What causes headaches?
There are thought to be over 300 causes of headaches and migraine and most fall into 3 categories:
- Cervicogenic headaches
- Migraine
- Tension type headache
It is possible to suffer from 2 or more different types of headaches at the same time.
Cervicogenic: these are headaches that originate from disorders of the neck. It is usually felt as a headache on one side of the head and often felt behind the eye. The pain is referred into the head from the bony structures or soft tissues of the neck due to the brain misinterpreting the true origin of the pain. Cervical headache is often precipitated by neck movement and/or sustained awkward head positioning and is often accompanied by restricted cervical range of motion, pain in the neck, shoulder, or arm usually on the same side as the headache.
Tension type: these headaches are the most common form of muscular (or myogenic) headaches and appear to involve the tightening or tensing of facial and neck muscles; they may radiate to the forehead.
Migraines: is the most common type of vascular headache. They are usually characterised by severe pain on one or both sides of the head, an upset stomach and occasionally disturbed vision. Migraines are more common in women and often hereditary.
What can you do for Headache?
Try to evaluate some of the possible contributing factors, several of which often exist together. Your physiotherapist can assist you with things you are unsure of:
- poor posture – especially if you tend to poke the chin forward or you are rounded through the upper back and shoulders. Try to have a curve in the lower back, and shoulder blades should be gently drawn back towards the spine, the neck should feel long and the chin slightly tucked in. A lumbar roll may help.
- neck and upper back stiffness– stiffness is often related to the ageing process and/or a sedentary lifestyle and/ or poor posture.
- muscle imbalances – these often develop due to poor postural positioning
- muscle weakness– this increases the work other muscles do – so they get tight, it also means you have less control of the movements occurring in your neck.
- muscle tightness – often caused by muscle imbalance and poor posture, try using a heat pack (e.g. a wheat bag where the muscles feel tight around the neck).
- previous neck trauma (e.g. whiplash)
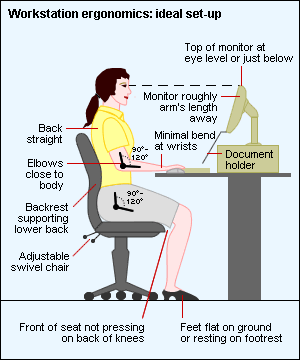
- inappropriate desk setup– your hips, knees and elbows should be at 90 degrees, if you are using a computer the screen should been at eye level.
- inappropriate pillow or sleeping postures – try to avoid sleeping on your stomach as this puts a lot of pressure on your neck. If you sleep on your side, try to have a pillow that keeps your neck in good alignment (i.e. not too high or too low).
- a sedentary lifestyle – try to keep active, even if it is 20-30 minutes of gentle walking or deep water running/ treading water.
- a lifestyle comprising excessive slouching, bending forwards or shoulders forwards activities – be careful of chairs (such as very soft couches) that you sink into. Try to stand up every 10-15 minutes, our bodies are not designed to sit for too long!
- stress – try to manage stress, regular exercise, an appropriate amount of sleep, plenty of water and fresh food will help, you can try massage, yoga or anything you find enjoyable to help manage stress. See your doctor if you feel you are still not managing your stress levels well.
How can Physiotherapy help?
Your physiotherapist will be able to assist you and give advice and education on how to improve on these factors as well showing you exercises and stretches to improve neck strength and flexibility. Your physio will also be able to provide ‘hands-on’ treatment to increase neck function, such as joint mobilisations, massage, acupuncture/dry needling, heat, ultrasound, postural taping or bracing and any other treatment that is specifically required. Your physio will also recommend consultation with your GP if physio treatment is not helpful for your type of headache.