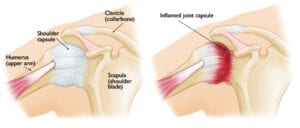
Often referred to as ‘frozen shoulder’, adhesive capsulitis refers to inflammation and scarring of the capsule which surrounds the shoulder joint.
How does it happen?
The exact reason why adhesive capsulitis develops is unknown. It can occur after trauma or surgery but can also develop spontaneously. It tends to occur in the middle aged or older populations and is believed to result from some form of irritation to the shoulder joint and its surrounding capsule. Irritation to the shoulder joint capsule results in an inflammatory response. This inflammation of the shoulder joint capsule is referred to as ‘capsulitis’. Associated with the capsulitis is the formation of adhesions or small scars between folds within the capsule. Consequently, the condition is referred to as adhesive capsulitis.
How does it feel?
The two main sensations felt with adhesive capsulitis are pain and a loss of movement in the shoulder. The pain may be aching, dull or stabbing, and is most frequently felt deep in the shoulder and over the outside of the upper arm. It is generally aggravated by almost all movements of the shoulder and arm, and its intensity or strength may vary from day-to-day depending on how much you use the arm. The pain is often strong enough to interfere with your normal activities and you may feel it at night when sleeping. The loss of movement in the shoulder results from the adhesions or scars forming within the joint capsule. These generally develop gradually resulting in a progressive rather than sudden loss in the range of motion in the shoulder. Stretching of these adhesions may aggravate your pain.
There are 3 stages of frozen shoulder:
- Stage one: The “freezing” or painful stage, which may last from six weeks to nine months, and in which the patient has a slow onset of pain. As the pain worsens, the shoulder loses motion.
- Stage two: The “frozen” or adhesive stage is marked by a slow improvement in pain but the stiffness remains. This stage generally lasts four months to nine months.
- Stage three: The “thawing” or recovery, when shoulder motion slowly returns toward normal. This generally lasts five months to 26 months.
What should you do?
If you have or suspect you have adhesive capsulitis you should seek the assistance of a physiotherapist or doctor as soon as possible to ensure an accurate diagnosis is made.
Initial management of adhesive capsulitis may include application of heat packs, massage therapy, gentle range of motion exercises, hydrotherapy (exercises performed in a heated pool) as well as taking anti-inflammatory and pain relieving medications.
Could there be any long-term effects?
Adhesive capsulitis usually gets better gradually over a period or months or years. Treatment can reduce this recovery time and can help provide pain relief and maximize function. Fortunately, once recovery does occur the long-term outlook is good, unless there is some other underlying condition affecting the shoulder, such as a tear of the rotator cuff.
Management of adhesive capsulitis with Physiotherapy
If the diagnosis of adhesive capsulitis is made, your physiotherapist will be able to provide you with an appropriate treatment program. This will most commonly be aimed at reducing your pain and improving your shoulder range of motion. It may involve the use of anti-inflammatory medications, electrotherapy treatment, and stretching, strengthening and range of motion exercises.
Surgical managment of frozen shoulder has mixed results. Hydrodilatation, where a combination of cortisone and saline are injected into the shoulder joint to dilate the capsule which reduce inflammation and pain, and hopefully increase range of motion since it stretches the restricted lining of the joint (capsule). If this is not successful the doctor may perform a manipulation under general anaesthetic to breakup the adhesions. Surgery to cut the adhesions (capsular release) may be warranted in prolonged and severe cases.
Usually however, adhesive capsulitis is a self limiting condition and can be managed with non-surgical intervention alone.